
Hi, I'm Sarah Mitchell. I've spent years researching metabolic health to help women reclaim their energy and balance their hormones naturally. Welcome to BioHealth Source.
You’ve been eating well. You’ve been walking after meals. You’ve been choosing the right carbohydrates. And yet — your blood sugar numbers are still higher than they should be.
If this sounds familiar, there’s a factor that most blood sugar guides completely ignore: stress.
Understanding how stress affects blood sugar is one of the most important — and most overlooked — pieces of the metabolic health puzzle. A single night of poor sleep or a demanding day at work can raise your fasting glucose by 20 to 30 mg/dL — completely independent of your diet. It explains why your numbers fluctuate even when your diet is consistent. And it points to a set of interventions that are just as evidence-backed as dietary changes.
In this guide, we’ll break down exactly how stress affects blood sugar, why this hormonal connection is so powerful, and — most importantly — what you can do to break the cycle.
If you’ve already worked through our guides on the prediabetes diet and the best protein sources for blood sugar, this guide completes the picture by addressing the hormonal factor that diet alone can’t fix.
What Is Cortisol — And Why Does It Affect Blood Sugar?
Cortisol is your body’s primary stress hormone — produced by the adrenal glands in response to physical or psychological stress. It’s often called the “fight-or-flight” hormone because its original purpose was to prepare your body for immediate physical action in response to danger.
Here’s what cortisol does in a stress response:
- It signals your liver to release stored glucose into the bloodstream — giving your muscles immediate fuel to fight or flee.
- It reduces insulin sensitivity — making your cells temporarily resistant to insulin so that glucose stays available in the blood for immediate use.
- It suppresses non-essential functions — including digestion, immune response, and reproductive hormones — to redirect energy toward survival.
This is an elegant and life-saving system when the stress is short-lived — a near-miss car accident, a physical threat, an acute emergency. Your blood sugar rises, you use the energy, and cortisol returns to baseline.
The problem is chronic stress.
In modern life, the stressors are rarely short-lived. Work pressure, financial anxiety, relationship conflict, sleep deprivation, social media overload — these are ongoing, low-grade stressors that keep cortisol elevated day after day. And chronically elevated cortisol means chronically elevated blood sugar — regardless of what you eat.
How Stress Affects Blood Sugar — The Science
The Hidden Spike: How Stress Affects Fasting Blood Sugar
One of the clearest ways how stress affects blood sugar is through your morning fasting numbers. Research from the Jackson Heart Study found that higher perceived stress levels were significantly associated with elevated fasting blood sugar — even after controlling for diet, exercise, and body weight.
This happens because cortisol signals the liver to release glucose overnight through a process called gluconeogenesis — the same process responsible for the Dawn Phenomenon, where blood sugar rises in the early morning hours before eating. Chronic stress amplifies this process, leading to persistently elevated fasting glucose even in people following a healthy diet.
For a complete breakdown of what your fasting numbers should look like and what causes them to rise, read our guide on blood sugar when fasting.
The Cortisol-Insulin Loop: How Stress Locks In Insulin Resistance
When cortisol is chronically elevated, it directly reduces insulin sensitivity — the ability of your cells to respond to insulin and absorb glucose efficiently. This is one of the most important mechanisms behind how stress affects blood sugar long-term — and one of the most frustrating, because it means dietary interventions alone are insufficient for people under chronic stress.
Research from Ohio State University found that chronic psychological stress is an independent risk factor for developing insulin resistance and type 2 diabetes — separate from dietary factors. This means that two people eating identical diets can have very different blood sugar responses if their stress levels differ significantly.
This loop also explains why chronic stress makes weight loss so difficult — elevated cortisol promotes fat storage, particularly around the abdomen, which further worsens insulin resistance. For a deeper understanding of how insulin resistance develops, read our guide on the early signs of insulin resistance.
Morning Highs: The Dawn Phenomenon Explained
One of the most confusing patterns for people managing blood sugar is waking up with elevated fasting glucose despite not eating overnight. This is the Dawn Phenomenon — and stress makes it significantly worse.
In the early morning hours (typically between 2 AM and 8 AM), your body naturally releases cortisol, growth hormone, and glucagon to prepare you for waking. These hormones signal the liver to release stored glucose — raising blood sugar before you’ve eaten a single thing.
For most metabolically healthy people, this rise is modest and quickly managed by insulin. But in people with insulin resistance or under chronic stress, the Dawn Phenomenon produces a significant morning spike — and chronically high evening cortisol from stress makes the overnight glucose release even more pronounced.
Understanding the Dawn Phenomenon is one of the key reasons why sleep and stress management directly impact your fasting blood sugar numbers.
How Stress Affects Blood Sugar After Meals
How stress affects blood sugar is not limited to the fasting state — it amplifies post-meal glucose spikes as well. When cortisol is elevated, the same meal that would produce a moderate glucose response on a calm day can produce a significantly higher spike on a stressful day.
This explains a common and confusing pattern: eating the exact same meal on two different days and seeing very different blood sugar responses. The meal didn’t change — the hormonal environment did.
To see how post-meal blood sugar should ideally look — and how stress changes that picture — read our guide on blood sugar after eating.
The Sleep-Cortisol-Blood Sugar Triangle
Sleep deprivation is one of the most powerful ways how stress affects blood sugar — and one of the most underestimated.
Research from the University of Chicago found that a single night of poor sleep reduced insulin sensitivity by up to 25%. Chronic sleep deprivation — consistently getting less than 7 hours per night — is one of the strongest independent predictors of prediabetes progression and type 2 diabetes risk.
The mechanism is direct: inadequate sleep raises cortisol, cortisol raises blood sugar, elevated blood sugar disrupts sleep quality further — creating a vicious cycle that is extremely difficult to break through diet alone.
The Stress-Blood Sugar Cycle — Why It’s So Hard to Break
Once you understand how stress affects blood sugar, the next question is: why is this cycle so hard to break?
High blood sugar caused by stress leads to energy crashes and fatigue — which increases stress. Stress disrupts sleep — which raises cortisol further. High cortisol drives sugar cravings — because your brain is seeking quick glucose for the perceived emergency. Giving in to those cravings spikes blood sugar further — which triggers more insulin, more fat storage, and more fatigue.
This cycle — stress → cortisol → high blood sugar → cravings → poor sleep → more cortisol — can continue indefinitely without targeted intervention.
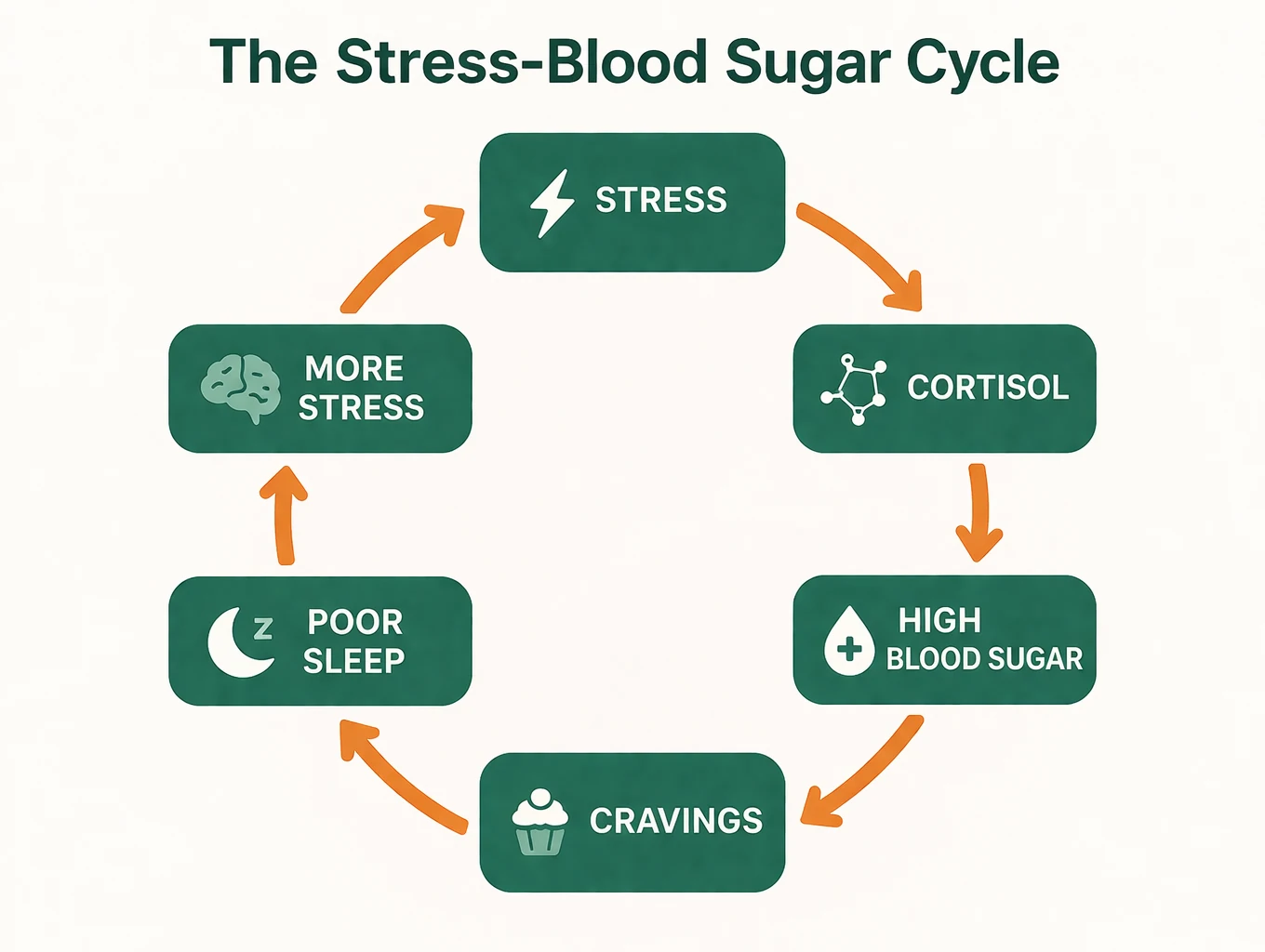
The good news is that the cycle is breakable. In the next section, we’ll walk you through 8 evidence-backed strategies that are simpler to apply than you might expect.
Calm vs. Stressed: How Your Body Responds Differently
The table below shows clearly how stress affects blood sugar response to the exact same meal:
8 Evidence-Backed Strategies to Lower Cortisol and Blood Sugar
1. Prioritize Sleep Above All Else

If there is one intervention with the greatest impact on how stress affects blood sugar, it is consistent, quality sleep. Aim for 7 to 9 hours per night. Keep a consistent sleep and wake schedule — even on weekends. The consistency of your sleep timing regulates your cortisol rhythm more effectively than sleep duration alone.
Practical steps: keep your bedroom cool (65–68°F is optimal), eliminate blue light exposure for 60 minutes before bed, avoid caffeine after 2 PM, and eat your last meal at least 2 to 3 hours before sleeping.
2. Walk After Meals — Even on Stressful Days
The post-meal walk is one of the most powerful dual-action interventions available — it lowers post-meal glucose directly through muscle glucose uptake AND reduces cortisol through physical movement and exposure to natural light.
Research consistently shows that even a 10-minute walk significantly reduces both cortisol and post-meal blood sugar. Read our complete guide on walking after meals benefits for the full science.
3. Practice Diaphragmatic Breathing

This is the fastest evidence-backed intervention for reducing acute cortisol — and it takes less than 5 minutes.
Slow, deep diaphragmatic breathing activates the parasympathetic nervous system — the “rest and digest” system that directly counteracts the cortisol response. Research shows that just 5 minutes of slow breathing (inhale for 4 counts, hold for 4, exhale for 6) significantly reduces cortisol and improves insulin sensitivity in the hours that follow.
This is particularly valuable before meals — taking 5 slow breaths before eating can meaningfully reduce the cortisol-amplified post-meal glucose spike.
4. Resistance Training
Building muscle is one of the most powerful long-term strategies for reversing how stress affects blood sugar. Resistance training improves insulin sensitivity, reduces baseline cortisol levels, and builds the metabolic reserve that buffers blood sugar fluctuations.
The key is consistency: 2 to 3 sessions per week produce measurable reductions in both fasting cortisol and fasting blood sugar within 4 to 8 weeks. Read our complete guide on exercises to reduce blood sugar levels for a practical plan.
5. Limit Caffeine — Especially on an Empty Stomach
Caffeine directly stimulates cortisol release. A morning coffee on an empty stomach can raise cortisol by 30% or more — amplifying the natural cortisol peak that already occurs in the early morning hours.
This doesn’t mean eliminating coffee. It means timing it strategically: waiting 60 to 90 minutes after waking before having your first cup, and eating before or with your coffee rather than after.
6. Magnesium Supplementation
Magnesium is one of the most evidence-backed supplements for reducing cortisol and improving blood sugar control simultaneously. Deficiency — which affects an estimated 50% of Americans — is directly linked to elevated cortisol, impaired sleep quality, and worsened insulin resistance.
Magnesium glycinate or magnesium malate (400 to 500 mg taken in the evening) has been shown to reduce fasting cortisol, improve sleep quality, and lower fasting blood sugar — making it one of the highest-value supplements for anyone managing how stress affects blood sugar.
🛒 Our Top Pick: Magnesium Glycinate is the most bioavailable form for managing the stress-cortisol connection without causing digestive upset. We recommend this high-absorption option for its purity and third-party testing.
7. Adaptogenic Herbs
Adaptogens are a class of natural compounds that help your body regulate its cortisol response — reducing the amplitude of the stress spike without suppressing cortisol entirely. Two have the strongest clinical evidence:
Ashwagandha (Withania somnifera) is one of the most studied adaptogens for cortisol reduction. Multiple randomized controlled trials have shown that ashwagandha supplementation significantly reduces serum cortisol, improves sleep quality, and reduces fasting blood sugar in people under chronic stress. A dose of 300 to 600 mg of root extract daily is the most studied protocol.
🛒 Research-Backed Option: Look for supplements containing the KSM-66 extract of Ashwagandha, which has the most robust clinical data for cortisol reduction. We recommend this KSM-66 option for its clinical-grade concentration.
Rhodiola Rosea has strong evidence for reducing stress-induced cortisol elevations and improving mental resilience under chronic stress. It works particularly well for stress related to cognitive overload — work pressure, mental fatigue, and anxiety — which are among the most common cortisol drivers in modern life.
Both adaptogens work best as part of a broader stress management strategy — not as standalone solutions.
8. Time-Restricted Eating
Eating within a consistent 8 to 10 hour window — for example, between 8 AM and 6 PM — reduces the metabolic stress placed on your digestive and hormonal systems, naturally lowering baseline cortisol and improving insulin sensitivity over time.
Time-restricted eating is not the same as aggressive caloric restriction — it simply aligns your eating pattern with your natural cortisol and insulin rhythm. Research consistently shows improvements in fasting blood sugar, insulin sensitivity, and sleep quality within 2 to 4 weeks of consistent practice.
3 Quick Stress Hacks for Blood Sugar — Starting Today
No time for a full routine? These three interventions take less than 15 minutes combined and produce immediate results:
Hack 1 — The 4-4-6 Breath (2 minutes)
Inhale for 4 counts. Hold for 4 counts. Exhale for 6 counts. Repeat 5 times before your next meal. This activates your parasympathetic nervous system within minutes — directly counteracting the cortisol response and improving insulin sensitivity before you even take your first bite.
Hack 2 — The 10-Minute Walk (10 minutes)
Walk within 30 minutes of finishing any meal — especially dinner. This single habit reduces both post-meal cortisol and post-meal blood sugar simultaneously. It’s the highest return-on-investment metabolic habit available. Read our complete guide on walking after meals benefits.
Hack 3 — The 10 PM Rule (0 minutes of effort)
Commit to being in bed with lights off by 10 PM at least 5 nights per week. Cortisol follows a strict circadian rhythm — staying up past 10 PM consistently disrupts the natural cortisol drop that should occur in the evening, keeping levels elevated into the night and raising your fasting blood sugar the next morning.
What Your Numbers Are Telling You
If you track your blood sugar regularly, understanding how stress affects blood sugar helps you interpret patterns that might otherwise seem random:
- Higher fasting blood sugar on mornings after poor sleep or high-stress days — cortisol-driven overnight glucose release
- Unexpectedly high post-meal readings despite eating well — cortisol amplifying insulin resistance in real time
- Blood sugar spikes without eating — acute stress events can raise blood sugar through cortisol release alone
- Difficulty bringing numbers down despite dietary changes — chronic stress may be undermining your dietary interventions
Our 7-day prediabetes meal plan shows exactly what to eat to keep these patterns under control.
These patterns are not failures of your diet or your willpower. They are the predictable, physiological consequences of chronically elevated cortisol — and they respond directly to the stress management interventions outlined above.
FAQ: How Stress Affects Blood Sugar
Can stress alone raise blood sugar without eating?
Yes — acute stress can raise blood sugar by 20 to 50 mg/dL through cortisol-driven liver glucose release, completely independent of food intake. This is one of the clearest examples of how stress affects blood sugar in real time.
How long does cortisol keep blood sugar elevated?
An acute stress response typically resolves within 1 to 2 hours as cortisol returns to baseline. Chronic stress keeps cortisol — and blood sugar — persistently elevated throughout the day, with the most pronounced effects in the morning due to the Dawn Phenomenon.
Does anxiety raise blood sugar?
Yes — anxiety triggers the same cortisol response as physical stress. Chronic anxiety is associated with significantly elevated fasting blood sugar and increased insulin resistance. Managing anxiety through breathing, movement, and sleep is therefore a legitimate blood sugar intervention. This is another example of how stress affects blood sugar through the same cortisol pathway.
Can reducing stress reverse prediabetes?
Stress management alone is unlikely to reverse prediabetes completely, but it is a necessary component of any comprehensive reversal strategy. Research shows that combining dietary changes — like those in our prediabetes diet guide — with stress reduction and sleep optimization produces significantly better outcomes than dietary changes alone.
What is the fastest way to lower cortisol naturally?
The fastest evidence-backed intervention is diaphragmatic breathing — 5 minutes of slow, deep breathing can measurably reduce cortisol within minutes. A 10-minute walk, brief meditation, or cold water on the face also produce rapid cortisol reduction through the parasympathetic nervous system.
Does cortisol cause weight gain around the belly?
Yes — chronically elevated cortisol promotes visceral fat accumulation specifically around the abdomen. This is both a symptom and a driver of insulin resistance, creating a cycle where belly fat worsens cortisol sensitivity and cortisol promotes further belly fat storage.
The Bottom Line
How stress affects blood sugar is not a secondary concern — it is a primary driver of metabolic dysfunction that operates independently of diet, exercise, and body weight.
Your blood sugar numbers reflect not just what you ate, but how well you slept, how much stress you experienced, and how effectively your nervous system is recovering between challenges.
The strategies in this guide — sleep optimization, post-meal walking, diaphragmatic breathing, resistance training, strategic caffeine timing, magnesium supplementation, adaptogenic herbs, and time-restricted eating — are not lifestyle luxuries. They are evidence-backed metabolic interventions that work on the same physiological mechanisms as dietary changes.
Start tonight: go to bed 30 minutes earlier than usual. Before your next meal, take 5 slow, deep breaths. After dinner, take a 10-minute walk. These three changes alone — applied consistently — will produce measurable improvements in your blood sugar numbers within weeks.
For the complete metabolic health picture, combine this guide with our prediabetes diet guide, our best protein sources guide, and our best low-glycemic carbohydrates guide.
“In all my years researching metabolic health, the pattern I see most consistently is this: people do everything right with food and still struggle. And when I dig deeper, the answer is almost always stress and sleep. Your body doesn’t separate ‘diet stress’ from ‘life stress.’ Cortisol doesn’t know the difference between a difficult meeting and a high-glycemic meal. It just raises your blood sugar either way. Managing stress isn’t soft advice — it’s metabolic medicine.”
— Sarah Mitchell
Sources & Scientific References
Ohio State University: Chronic Stress and Insulin Resistance. Research demonstrating how psychological stress triggers inflammatory responses that act as an independent risk factor for Type 2 Diabetes.
University of Chicago: Sleep Deprivation and Insulin Sensitivity. A landmark study showing that just one night of restricted sleep can reduce insulin sensitivity by up to 25%.
Cleveland Clinic: Cortisol and Glucose. A medical breakdown of why stress hormones signal the liver to release extra sugar into the bloodstream.
Harvard T.H. Chan School of Public Health: Stress and Health. Comprehensive analysis of how chronic stress disrupts metabolic hormone regulation.
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK): Insulin Resistance and Prediabetes. Clinical breakdown of how hormones like cortisol interfere with glucose uptake in muscle and liver cells.
National Center for Biotechnology Information (NCBI): Stress, Cortisol, and Glycemic Control. A study detailing how the “fight-or-flight” response impacts blood glucose levels.
Medical Disclaimer: The information provided on BioHealth Source is for educational and informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional before making significant changes to your diet, exercise routine, or if you have questions regarding a medical condition.
Affiliate Disclosure: This post may contain affiliate links. If you click on one of these links and make a purchase, we may receive a small commission at no extra cost to you. This helps support our research and content creation. We only recommend products we truly believe in.

